Keywords
Bilateral subclavian artery stenosis, vertebrobasilar insufficiency, shock, pseudoshock, peripheral vascular disease, vasopressors
Abstract
Introduction: Subclavian artery stenosis (SAS) is a manifestation of peripheral artery disease (PAD). Presentation varies, ranging from arm claudication and muscle fatigue to symptoms which reflect vertebrobasilar hypoperfusion, among which are syncope, ataxia and dysphagia. Although rare, severe bilateral SAS can exist and present as refractory hypotension. We describe a case of bilateral SAS masquerading as circulatory shock, or rather ‘pseudoshock’.
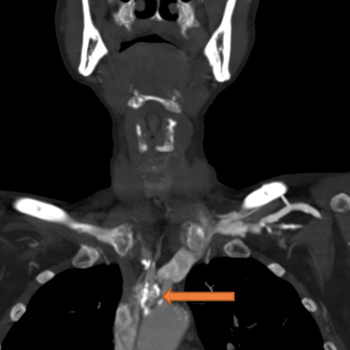
Case Description: A 59-year-old female patient presented to the emergency department with complaints of dark stools. She was anaemic and hypotensive and therefore suspected to have an acute gastrointestinal bleed (GIB) with resultant haemorrhagic shock. Her hypotension was unresponsive to fluid resuscitation and blood transfusions. Bilateral upper extremity radial artery catheters confirmed low blood pressures. After her blood pressure failed to improve despite the addition of several vasopressors, a femoral artery catheter (FAC) was placed, which revealed significant hypertension discordant with the hypotension measured by the radial artery catheters. Review of CT angiography of the upper extremities revealed the presence of bilateral SAS which was deemed to be the aetiology of the falsely low blood pressure.
Discussion: SAS should be suspected in patients with lower extremity PAD or a blood pressure (BP) differential of 15 mmHg or more between arms. When bilateral subclavian arteries are stenosed, this difference in BP may be concealed, making lower extremity BP measurements, as seen in non-invasive tests such as ankle brachial index (ABI) tests or through more invasive procedures such as FAC placement, critically important.
Conclusion: Bilateral SAS may present as pseudo-hypotension. In cases of refractory shock of unclear aetiology, especially in patients with known PAD, a high index of suspicion is warranted for ‘pseudoshock’ secondary to severe vascular stenosis. Comparison of upper and lower extremity BP via invasive arterial catheters or non-invasive ABI tests can aid in the diagnosis of bilateral SAS.
References