ABSTRACT
Endoscopic retrograde cholangiopancreatography (ERCP) is a diagnostic and therapeutic tool for pancreaticobiliary diseases. Like every other procedure, ERCP can lead to complications that include pancreatitis, cholecystitis, perforation, and rarely, retroperitoneal hematoma. We present a case of post-ERCP acute hemorrhagic pancreatitis resulting in retroperitoneal hematoma and sequelae of unilateral hydronephrosis and ileus. The patient was treated supportively and had good clinical improvement with resolution of hydronephrosis, ileus and more importantly tolerating oral diet without further episodes of abdominal pain.
LEARNING POINTS
- The most common complications of endoscopic retrograde cholangiography are acute pancreatitis and hemorrhage. In high-risk patients, acute pancreatis can be prevented with rectal non-steroidal anti-inflammatory suppository before the procedure.
- Occurrence of Grey-Turner or Cullen sign should prompt immediate search for retroperitoneal hematoma especially in the setting of acute hemorrhagic pancreatitis.
- Apart from hemodynamic instability or compressive symptoms, retroperitoneal hematoma can also cause complications due to inflammatory reactions resulting in hydronephrosis or ileus.
KEYWORDS
Endoscopic retrograde cholangiopancreatography, Retroperitoneal hematoma, Hemorrhagic pancreatitis, hydronephrosis
INTRODUCTION
Endoscopic retrograde cholangiopancreatography (ERCP) is a procedure that combines X-Ray and endoscopy and has been used for more than 40 years. ERCP has emerged as a crucial tool to investigate and treat conditions affecting the bile ducts and pancreas. This minimally invasive procedure allows physicians to visualize and manipulate the biliary and pancreatic ducts, providing valuable insights into various disorders[1,2]. While ERCP offers invaluable benefits, it is not without potential complications. Acute pancreatitis is the most common complication with an incidence of 3.5 to 9.7 percent, with severe pancreatitis accounting for 0.3 to 0.8% of cases[3,4]. There are very rare reports of acute hemorrhagic pancreatitis post ERCP. We present a case of acute hemorrhagic pancreatitis resulting in retroperitoneal hematoma. The aim is to shed light on one of the rarest complications of this procedure that clinicians and patients must be aware of[5,6]. By understanding the intricacies of ERCP and its complications, healthcare professionals and patients can work together to make informed decisions and optimize patient safety.
CASE DESCRIPTION
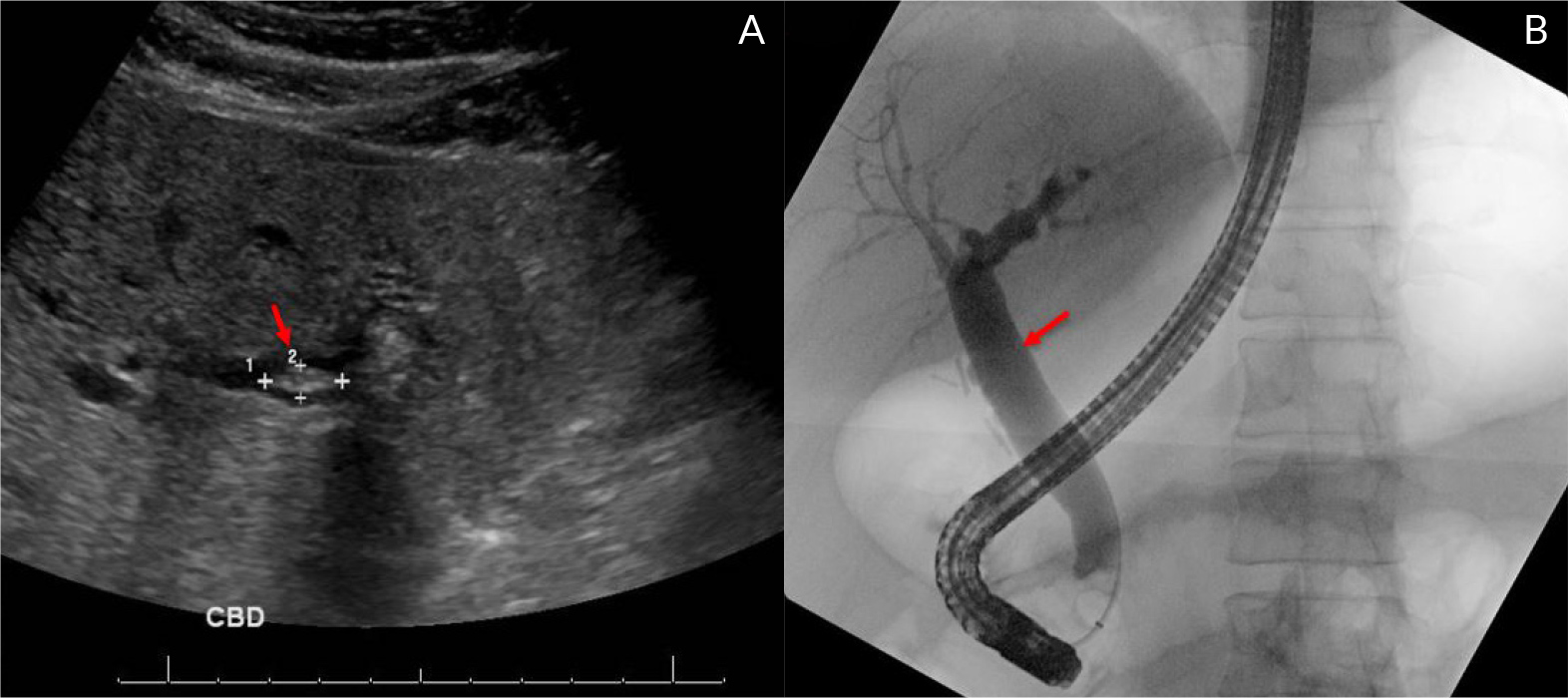
A 41-year-old male presented to the emergency room with acute onset of nausea, vomiting and abdominal pain of 3 days duration. His medical history included nephrolithiasis. Surgical history included cholecystectomy for choledocholithiasis at the age of 14. On presentation, he was in acute distress due to pain, with vital signs showing blood pressure (BP) 153/109 mmHg, heart rate (HR) 110 beats/minute and absence of fever. Physical examination revealed right upper quadrant tenderness. Laboratory work-up revealed white blood cell count of 8,400 cells/Ul, hemoglobin 15 g/dl, lipase 38 U/l, aspartate aminotransferase (AST) 608 U/l, alanine aminotransferase (ALT) 1,559 U/l, alkaline phosphatase (ALP) 276 U/l, total and direct bilirubin of 3.4 mg/dl and 2 mg/dl respectively. Computed tomography (CT) of the abdomen and pelvis with contrast revealed mild biliary dilation, and ultrasound revealed common bile duct (CBD) dilated to 9 mm with a potential stone (Fig. 1A). A diagnosis of choledocholithiasis was made and he underwent ERCP which revealed dilated CBD of 15 mm on fluoroscopy with a distal CBD stricture (Fig. 1B). Stone extraction was performed with balloon sweep and a 3 mm stone along with sludge was removed.
Figure 1. A) Ultrasound of the right upper quadrant showing a dilated common bile duct with intraductal echogenic foci consistent with stone (red arrow). B) Fluoroscopy imaging during ERCP showing dilated CBD measuring 15mm (red arrow)
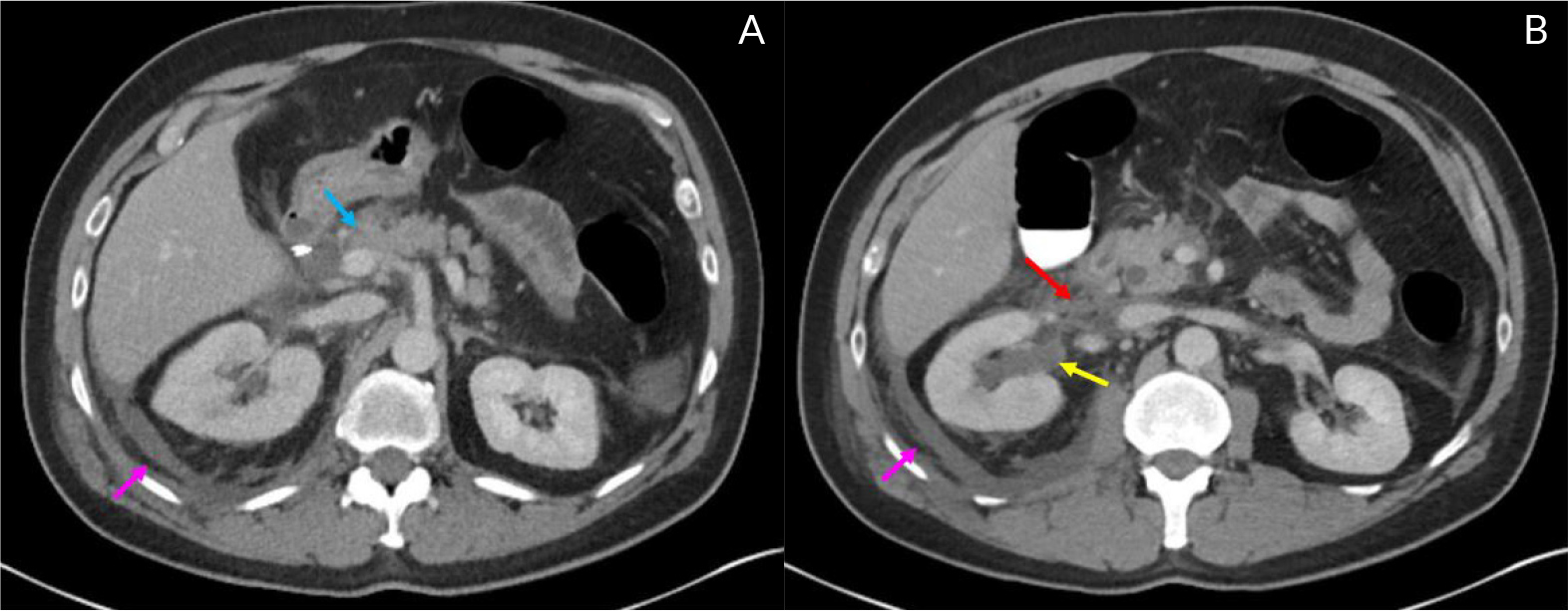
A few hours after ERCP, the patient developed new onset epigastric pain, radiating to his back with a pain intensity of 10/10. Examination revealed distended abdomen and epigastric tenderness. Laboratory studies revealed lipase 1,356 U/l, AST 178 U/l, ALT 609 U/l, alkaline phosphatase 237 U/l, total bilirubin 3 mg/dl, and direct bilirubin 1.6 mg/dl. He was diagnosed with post-ERCP pancreatitis and was started on supportive care. Despite being on a patient-controlled analgesia pump (PCA) of hydromorphone, his pain was not well controlled, and he developed dysuria with right costovertebral angle tenderness, prompting repeat imaging. CT of the abdomen and pelvis revealed peripancreatic inflammatory stranding of pancreatic head and neck with pancreatic swelling and extensive soft tissue swelling and inflammatory changes in the retroperitoneum extending to the presacral region and left pelvic region. Persistent CBD dilation of 1 cm and choledocholithiasis were apparent. There was also new right hydronephrosis with inflammatory changes around the right ureteropelvic junction (Fig. 2). A follow-up renal ultrasound to evaluate the hydronephrosis did not reveal any stone in the right ureter and serum creatinine was 0.7 mg/dl. Given the persistent diagnosis of choledocholithiasis, he underwent repeat ERCP on post operative day 4. Balloon sweep did not yield any stone and a 10 Fr 7 cm plastic CBD stent was placed across the edematous ampulla and distal CBD stricture.
Figure 2. Computed tomography (CT) of the abdomen with contrast-axial view showing A) swelling and peripancreatic inflammation with fat stranding around the head and neck of pancreas (blue arrow); inflammatory changes in the retroperitoneal region (pink arrow) B) right hydronephrosis (yellow arrow), inflammatory changes around the right ureteropelvic junction (red arrow) and retroperitoneal region (pink arrow)
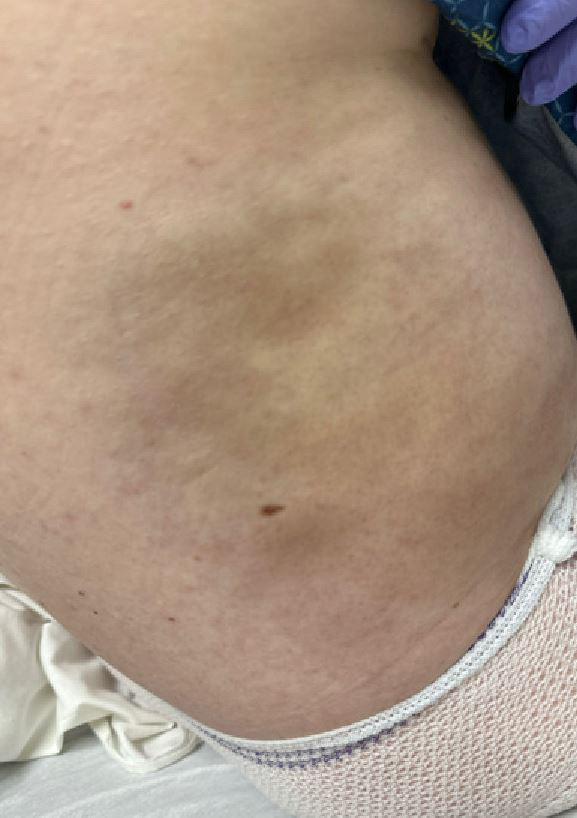
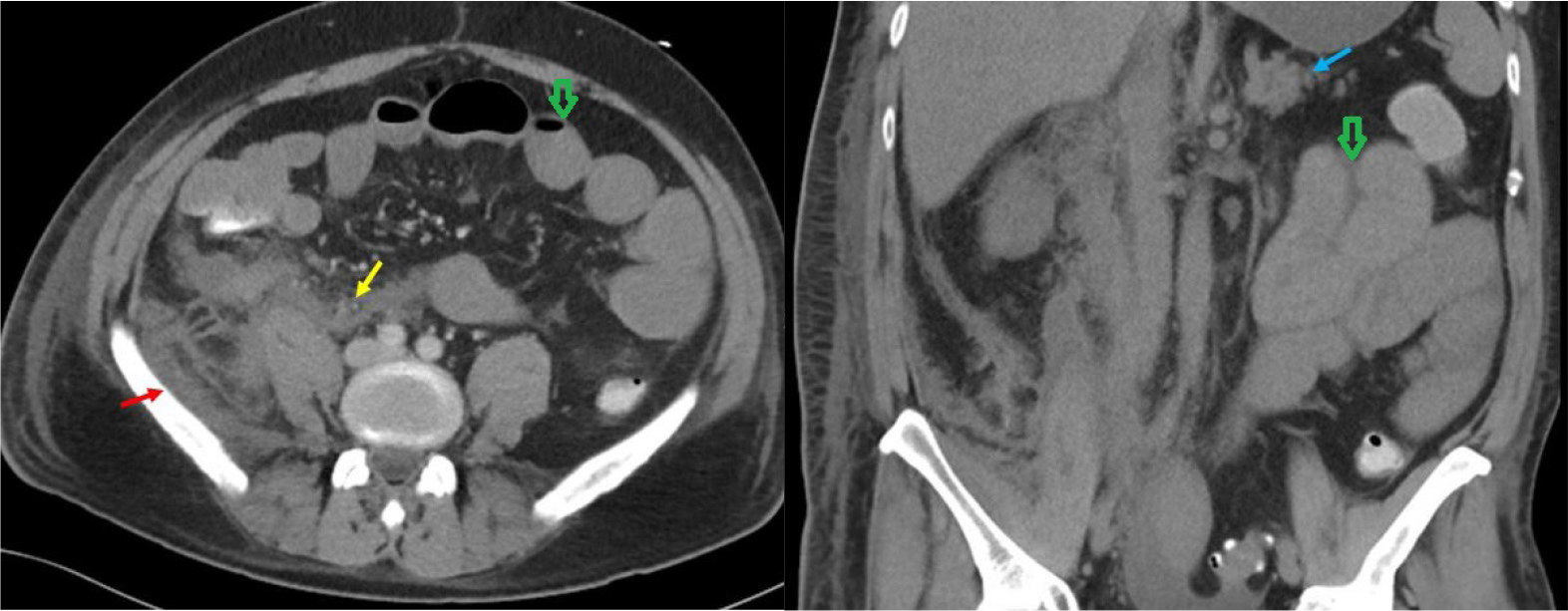
Two hours after the procedure, the patient complained of severe abdominal pain. Examination revealed a distended abdomen, bluish discoloration of the right flank suspicious for Grey-Turner sign and generalized tenderness (Fig. 3). Vital signs revealed BP 135/86 mmHg, HR 108 beats/minute and absence of fever. A third CT of the abdomen and pelvis showed high density fluid in the lesser sac extending into the right retroperitoneum concerning for retroperitoneal hematoma. The hemorrhage appeared to surround the pancreatic head, possibly indicative of hemorrhagic pancreatitis (Fig. 4). No evidence of pancreatic necrosis or active bleeding was found. There were also multiple loops of dilated small bowel with air-fluid level indicative of ileus. Laboratory work-up showed Hgb 12.8 g/dl, ALT 142 U/l, AST 36 U/l, lipase 26 U/l and total bilirubin 1.2 mg/dl. Given his imaging and clinical findings, the patient was transferred to an intensive care unit for close monitoring and more advanced care if needed.
During his ICU stay, the patient remained hemodynamically stable and did not need any blood transfusion. His hemoglobin level dropped to 10.8 mg/l before stabilizing. Due to his stable retroperitoneal hematoma and his hemodynamic stability, no surgical intervention was warranted. He was started on stomach decompression with bowel rest for ileus, IVF and pain control. He slowly showed clinical improvement, started having bowel movements, and tolerated oral feeds. He was discharged on day 21 in stable condition to follow up with the gastroenterologist for removal of the CBD stent in 2 months.
Figure 3. Photograph of the patient’s right flank showing area of ecchymosis consistent with Grey-Turner sign
Figure 4. CT of the abdomen and pelvis with contrast A) Axial view showing hematoma in the retroperitoneal (red arrow) and lesser sac (yellow arrow) with dilated bowel loop (green arrow) B) Coronal view showing extensive inflammation with hematoma on the right side and portion of pancreas (blue arrow) and dilated bowel loop (green arrow)
DISCUSSION
Endoscopic retrograde cholangiopancreatography (ERCP) is considered a safe procedure, but complications can infrequently occur. The most common complications are acute pancreatitis and hemorrhage from the sphincterotomy site. Acute pancreatis is the most common complication[2,7]. The pathogenesis is suspected to involve mechanical, thermal, or chemical injury, resulting in edema of the pancreatic duct orifice or duct itself. Post-ERCP pancreatitis is defined as new onset or worsening of the pre-existing abdominal pain along with increase in lipase or amylase more than 3 times the upper normal limit lasting for more than 24 hours after ERCP and resulting in prolongation of a planned admission[7]. Our patient who underwent ERCP presented with acute choledocholithiasis and developed worsening abdominal pain associated with elevated lipase and prolonged hospitalization, thereby meeting the criteria of post-ERCP pancreatitis. The use of non-steroidal anti-inflammatory drugs like indomethacin suppository or diclofenac is advised before the procedure to prevent this complication in high-risk individuals[7,8].
Though most post ERCP pancreatitis cases are mild, there is a low incidence of severe disease. Post-ERCP hemorrhagic pancreatitis or the occurrence of retroperitoneal hematoma as its sequela are rarely reported. Acute pancreatitis is more evident on imaging a few days after symptom onset[9]. We suspect that our patient developed acute hemorrhagic pancreatitis following the initial ERCP but this was more apparent on imaging 4 days later, with focal involvement of the head and neck.
Retroperitoneal hematoma following ERCP is an extremely rare occurrence. It typically arises from vascular injury during cannulation, sphincterotomy, or passage of instruments through the papilla[10]. The vascular structures in the vicinity, such as the pancreaticoduodenal artery or its branches, can be inadvertently injured, leading to bleeding into the retroperitoneal space. Extensive literature search revealed only 1 case of retroperitoneal hematoma of unknown source post ERCP in a liver transplant patient[11]. Our patient had classic Grey-Turner sign with imaging revealing retroperitoneal hematoma. The suspected source was hemorrhagic pancreatitis as evidenced on final CT by the hemorrhage in the right retroperitoneal space in continuity to the pancreas.
In this case, the patient had abdominal pain and Grey-Turner sign following the second ERCP procedure. Imaging revealed a retroperitoneal hematoma, causing compression on the adjacent structures, including the ureter, leading to hydronephrosis. Retroperitoneal hematomas can exert pressure on surrounding organs and structures, leading to complications such as hydronephrosis, urinary obstruction, or even renal failure[12,13]. We suspect that more than a pressure effect, the inflammatory reaction at the right ureteropelvic junction caused edematous changes, blocking the right ureter resulting in retrograde right hydronephrosis. The inflammatory process in the ileus in our patients is suspected to be the same as that reported by Drew[14]. The suspected succession of events is represented in figure 5.
Prompt recognition and management of retroperitoneal hematoma are crucial to prevent complications. Conservative management with close monitoring, bed rest, and supportive care are often prescribed for stable patients with small hematomas. However, in cases of expanding or symptomatic hematomas, intervention may be necessary. Options for intervention include arterial embolization or surgical exploration and evacuation of the hematoma[13,15].
Treatment of hydronephrosis secondary to retroperitoneal hematoma involves relieving the obstruction and addressing the underlying cause[12,16]. While treatment of ileus is the same as for other causes, bowel rest and stomach decompression are also necessary until the inflammation subsides. Our patient responded well to supportive care leading to resolution of both hydronephrosis and ileus.
This case report emphasizes the importance of recognizing and managing rare complications of ERCP such as retroperitoneal hematoma and subsequent hydronephrosis and ileus due to post ERCP acute pancreatitis. Prompt identification, close monitoring, and timely intervention are crucial in preventing further morbidity and optimizing patient outcomes. Healthcare providers performing ERCP should maintain a high index of suspicion for such complications and be prepared to promptly initiate appropriate management strategies.