ABSTRACT
Livedoid vasculopathy (LV) is a rare clinical condition presenting as painful lesions mostly on the lower extremities. We present a case of LV with peripheral neuropathy in a young man initially misdiagnosed and treated for cellulitis. He was started on aspirin, pentoxifylline and apixaban immediately after the diagnosis of LV. However, pain management was a real challenge for the clinicians. Hence, he was later treated with epoprostenol and amlodipine for vasodilation, steroids for any possible inflammation, and antibiotics to treat superimposed infection. Irrespective of all the above, his pain was uncontrollable, and he finally received ketamine infusions along with narcotics, achieving better pain control. Various studies support the use of intravenous immunoglobulin and anti-TNF agents for pain relief in idiopathic and secondary LV. Intermittent low-dose dabigatran has also been found to be effective in the maintenance of remission in LV. However, no large studies have yet been conducted to confirm the efficacy of these medications.
LEARNING POINTS
- Early initiation of treatment with antiplatelets and anticoagulants is recommended to prevent the progression of livedoid vasculopathy (LV).
- Anti-TNF agents can be tried in refractory LV for rapid relief of pain.
- Intravenous immunoglobulin has been shown to be effective for the resolution of pain and improvement of neuropathic symptoms especially in LV refractory to immunosuppressive agents.
KEYWORDS
Livedoid vasculopathy, peripheral neuropathy, pain management
INTRODUCTION
Livedoid vasculopathy (LV) is an extremely rare disease which presents initially as painful, erythematous or purpuric plaques which may eventually ulcerate [1-3]. LV has an estimated prevalence of 1 in 100,000 in North America, predominantly in females [4]. Appropriate and timely initiation of treatment is recommended to reduce pain and prevent complications [5].
CASE DESCRIPTION
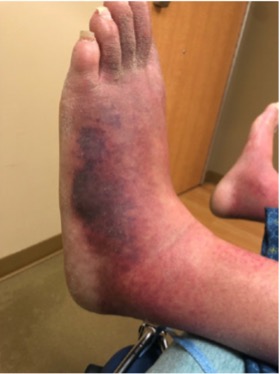
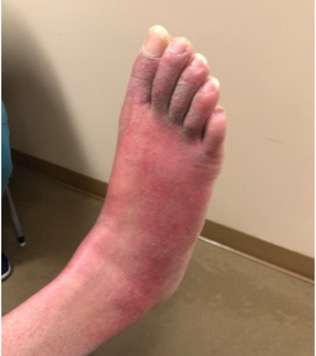
A 22-year-old man with a history significant for uncontrolled type 1 diabetes mellitus (HbA1C 13.2%) and spontaneous pneumothorax presented to the emergency department with extremely painful bilateral lower extremity swelling of 2 weeks duration. On presentation, he was haemodynamically stable and afebrile, but was in severe distress secondary to pain. Examination revealed a tall young man with marfanoid features and erythematous bilateral lower extremities swollen up to the knees, with blisters and violaceous lesions on the lateral aspects of the feet (Fig. 1 and 2).
Hyperaesthesia was also noted. Initial work-up revealed an elevated erythrocyte sedimentation rate (ESR) of 36 mm/hr and C-reactive protein of 53.9 mg/l without leucocytosis. Arterial and venous Doppler scans were unremarkable. The patient was empirically treated with multiple antibiotics for cellulitis without any clinical improvement. Further, a differential diagnosis of vasculitis versus connective tissue disease was considered, but serological work-up including ANA, ANCA, Rh factor and APLA antibodies was negative. Also, work-up for thrombophilia including factor V Leiden mutation and prothrombin gene mutation returned negative. Hence, biopsy along with direct immunofluorescence was performed which revealed fibrin formation in small vessels positive for IgM and C3. The patient was treated with aspirin, pentoxifylline, apixaban and pregabalin along with oxycodone for pain management without much clinical improvement, especially regarding pain control.
The patient was readmitted twice for pain crises which were further treated with epoprostenol and amlodipine along with steroids to reduce inflammation initially, and finally ketamine infusion with transcutaneous electrical nerve stimulation which resulted in adequate pain control.
Figure 1. Erythematous violaceous plaques on the lateral aspect of the left foot
Figure 2. Erythematous right foot with poor demarcation, appearing similar to cellulitis of the foot
DISCUSSION
Livedoid vasculopathy is a painful, ischaemic vaso-occlusive disease of the lower extremities associated with micro thrombosis of the vessels in the dermis [1, 2]. It usually presents as extremely painful ulcers of the lower extremities which start around the ankles [1-3]. Histopathology demonstrates the presence of intraluminal thrombosis in the dermis, and sometimes endothelial proliferation and subintimal hyaline PAS-positive degeneration [3]. When clinical findings and histopathology are indeterminate, direct immunofluorescence helps to reach the diagnosis. The deposition of a combination of multiple immune reactants either in the blood vessels or in the dermo-epidermal junction has been demonstrated in previous studies [6]. Among the immune complex deposits, C3 complement–IgM complex was the most common combination observed, as seen in our patient [6]. LV can be secondary to thrombophilia, connective tissue disease, hypercoagulable states or malignancy [5, 7]. It has been reported to be idiopathic in 20% cases [5, 7].
Soulages et al. demonstrated that the association of peripheral neuropathy with LV can be either due to occlusion of small nerve vessels causing mononeuropathy multiplex or due to peripheral neuropathy from autoimmune disease [2].
Treatment options include anticoagulants, antiplatelets, anabolic steroids, thrombolytics, hyperbaric oxygen, intravenous immunoglobulins and UV light [1]. Good clinical outcomes were observed with all the above therapies, with anticoagulants being the most commonly used treatment [1, 5, 8][1, 5, 8]. Antiplatelets like aspirin, pentoxifylline and dipyridamole remain the first-line therapeutic options along with rivaroxaban, warfarin and low-molecular-weight heparin in associated thrombophilia [1, 5]. Second-line therapeutic options include anabolic steroids, intravenous immunoglobulins and hyperbaric oxygen [5, 9]. Third-line options in resistant cases include hydroxychloroquine in systemic lupus erythematosus and APLA, oral colchicine or dapsone in vasculitis [5]. Other options in resistant cases include multivitamins, cyclosporin A, cyclophosphamide, azathioprine, systemic phototherapy and vasodilators like nifedipine [5]. Also, previous literature supports the addition of alprostadil to the treatment regime in preventing recurrence [10].
A study conducted to determine the efficacy of anti-TNF agents in the management of LV revealed a 34.3% reduction in pain after 12 consecutive weeks of etanercept therapy [11]. Anti-TNF agents including etanercept and adalimumab have been found to be effective in primary and secondary LV especially for the rapid relief of pain [11, 12].
Plasminogen activator inhibitor-1 is observed to have a potential aetiological role in the pathogenesis of LV. Therapies targeting PAI-1 can pave the way for further studies in treating refractory LV [13]. Song et al. have published a case report on sulodexide, which is a highly purified mixture of glycosaminoglycan including dermatan sulfate and low-molecular-weight heparin proven to be effective in the treatment of LV [14]. Intermittent low-dose dabigatran has also been proven to be effective in the maintenance of remission in LV [15]. Tofacitinib, a pan Janus-kinase inhibitor which inhibits T-cell survival and regulation, was also used with success in refractory LV [16].
In a systematic review performed by Gao et al., intravenous immunoglobulin therapy was found to be effective for pain relief as well as neurological symptoms [17]. It is therefore an effective alternative for immunomodulators and immunosuppressive agents in treatment failure [17]. IVIG therapy can also be used for patients who do not tolerate long-term immunosuppressive agents [17].
Although the pathogenesis of LV is unclear, demonstration of immunoreactant deposition confirms that LV is associated with pathologies involving immune and inflammatory pathways. Strong associations with autoimmune disease have been found in previous studies. Hence anti-TNF agents and IVIG therapy which interfere with the inflammatory response can be used for the management of pain in refractory LV. Further large-scale studies are needed to determine the treatment guidelines for the management of pain in LV.