ABSTRACT
Fever of unknown origin remains a diagnostic challenge. Aortitis, defined as inflammation of the aorta, has multiple infectious and non-infectious causes.
We report the case of an elderly woman with vertigo and bilateral hearing loss, presenting with fever of unknown origin. Blood tests were remarkable for leucocytosis with neutrophilia, elevation of C-reactive protein and the erythrocyte sedimentation rate, and positive antinuclear antibodies and rheumatoid factor, and an unremarkable search for multiple infectious causes of fever. During admission the patient developed a bilateral red eye. Abdominal and chest computed tomography was performed and demonstrated signs of aortitis.
Due to the coexistence of aortitis, ocular inflammation, vertigo and bilateral hearing loss in a patient with persistent fever and elevation of inflammatory parameters, a presumptive diagnosis of Cogan’s syndrome was made, with improvement after initiation of steroid therapy.
LEARNING POINTS
- Fever of unknown origin is a diagnostic challenge with an extensive list of possible causes.
- The coexistence of fever, aortitis, ocular and vestibulo-cochlear symptoms should raise the suspicion of Cogan’s syndrome.
- Steroid therapy is the first-line treatment for Cogan’s syndrome.
KEYWORDS
Aortitis, Cogan’s syndrome, fever of unknown origin
INTRODUCTION
Fever of unknown origin (FUO), defined as a temperature of 38.3°C (101°F) or higher for more than 3 weeks, without an established diagnosis despite at least 1 week of investigation in the hospital including thorough history-taking, physical examination and basic investigations, remains a diagnostic challenge, with an extensive list of possible causes.
Aortitis is the term used to describe inflammation of the aorta [1]. The most common causes of aortitis are non-infectious, and include large vessel vasculitis, such as Takayasu arteritis and giant cell arteritis, and autoimmune diseases, such as rheumatoid arthritis, systemic lupus erythematosus and Behçet’s disease.
CASE DESCRIPTION
An 80-year-old Caucasian woman presented to the emergency department with a 1-week history of fever, fatigue, cough and haemoptysis. Her past medical history was notable for hypertension, depression and vertigo, accompanied by bilateral hearing loss. At admission, blood tests demonstrated leucocytosis (21,900/µl) with neutrophilia (88.9%) and elevation of C-reactive protein (CRP) (346.4 mg/l). Chest x-ray demonstrated a right lower lobe infiltrate, while SARS-CoV-2 and influenza A and B PCR were negative. A diagnosis of community-acquired pneumonia was made, and ceftriaxone and azithromycin therapy was instituted. After 6 days of antibiotic therapy, the fever and elevation of inflammatory parameters persisted. Blood and urine cultures were collected, and antibiotic therapy was escalated to piperacillin-tazobactam plus gentamicin. Due to persistence of fever and elevation of inflammatory parameters after 4 days of piperacillin-tazobactam plus gentamicin, new blood and urine cultures were collected and antibiotic therapy was escalated to meropenem.
On the 10th day of admission, the patient developed a bilateral red eye, with signs of conjunctivitis and chemosis.
The search for infectious causes was unremarkable, with repeated negative blood and urine cultures, negative serologies forTreponema pallidum, Leptospira, Brucella, Borrelia burgdorferi, Coxiella burnetii, Rickettsia conorii, HIV, hepatitis B and C and negative interferon gamma release assay (IGRA). A transthoracic echocardiogram was normal. The erythrocyte sedimentation rate (ESR) was elevated and antinuclear antibodies (ANA) and rheumatoid factor (RF) were positive.
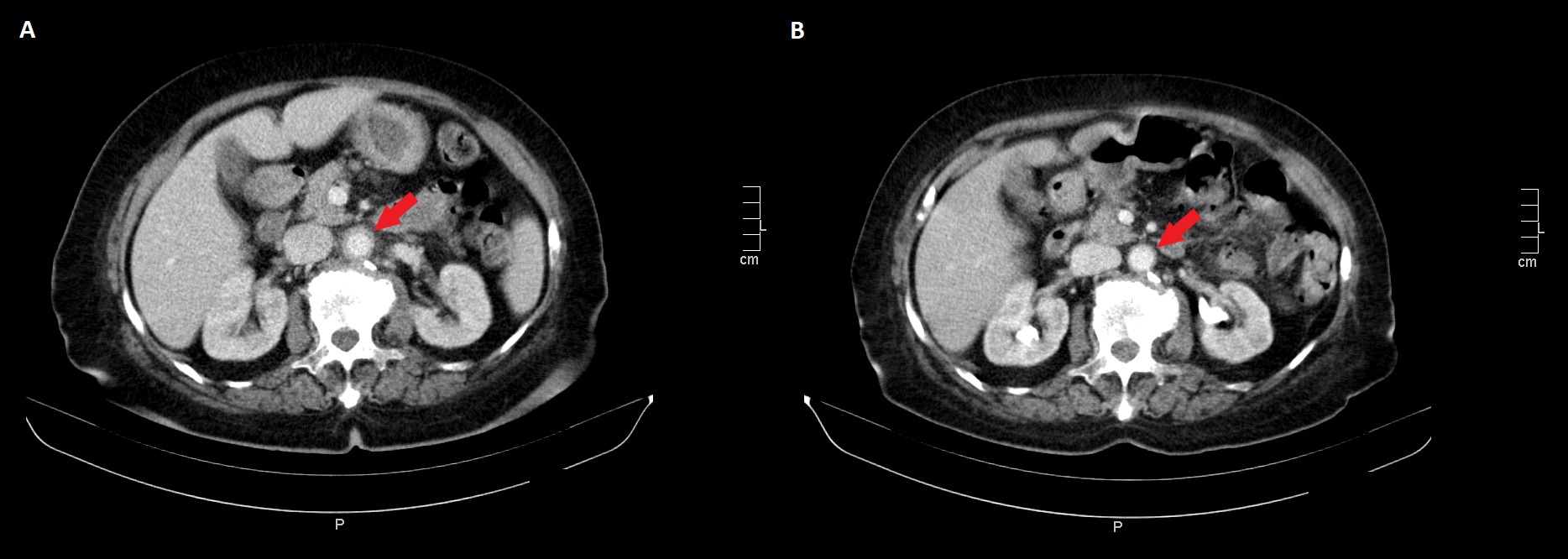
Abdominal and chest computed tomography (CT) was performed and demonstrated circumferential parietal thickening of the thoracic and superior abdominal aortic wall, suggestive of vasculitis (Fig. 1A).
Due to the coexistence of aortitis, ocular inflammation, vertigo and bilateral hearing loss in a patient with persistent fever and elevation of inflammatory parameters, a presumptive diagnosis of Cogan’s syndrome was made. Steroid therapy with prednisone 1 mg/kg daily was initiated, with resolution of fever, vertigo and laboratory abnormalities, and improvement of imaging findings of aortitis (Fig. 1B).
Figure 1. (A) Computed tomography showing parietal thickening of the superior abdominal aortic wall, suggestive of aortitis. (B) Improvement of parietal thickening of the superior abdominal aortic wall after steroid therapyyl prednisolone.
DISCUSSION
Cogan’s syndrome is a rare autoimmune systemic vasculitis characterized by intraocular inflammation and vestibulo-auditory disfunction[2]. The average age at disease onset is 29 years, but although less common, there have been several descriptions of late-onset disease, as in the case presented [3]. The onset of disease is preceded by respiratory tract infection in approximately 30% of cases. In 25% of patients, the eye and the ear are involved simultaneously and in another 10%, the disease is complicated with systemic vasculitis [2]. There are no specific markers for Cogan’s disease, but leucocytosis, anaemia, thrombocytosis, and elevated ESR and CRP are common findings and, in some cases, rheumatoid factor and antinuclear antibodies are detected, as in the case presented [2].
Aortic imaging is essential for both diagnosis and follow-up of patients with Cogan’s syndrome, and while CT and magnetic resonance imaging are most often used to detect the diffuse aortic wall thickening suggestive of inflammation, PET/CT has recently been found useful in revealing the degree of inflammation and helping to decide the intensity of therapy [4]. In this case, CT was enough to diagnose aortitis and follow-up the response to therapy.
Treatment of systemic disease consists of systemic steroids (high-dose prednisone 1–1.5 mg/kg daily until hearing improves, typically after 2–3 weeks, followed by a slow taper and continuation of treatment for 2–6 months), with or without steroid-sparing agents, such as cyclophosphamide, azathioprine and methotrexate [5]. In this case, systemic steroids alone led to resolution of all manifestations of Cogan’s syndrome. Infliximab is an alternative when steroids fail or if there is severe ocular, cochlear or systemic involvement [6].
Aortitis should be considered as a possible aetiology of FUO, and while giant cell arteritis is the most common large vessel vasculitis in elderly women, Cogan’s syndrome, despite being a rare cause of FUO, should be suspected when the patient presents with ocular and vestibulo-cochlear involvement. Early recognition of this entity is crucial in reducing the risk of complications through the initiation of treatment.