ABSTRACT
Persistent left superior vena cava (PLSVC) is a congenital venous abnormality, characterized by an enlarged coronary sinus, in most cases without haemodynamic consequences. We report the case of a patient with systolic heart failure undergoing implantation of a defibrillator lead through a PLSVC which was diagnosed at the moment of implantation.
LEARNING POINTS
- Persistent left superior vena cava (PLSVC) can be incidentally diagnosed during a procedure such as a left-sided central venous line or pacemaker implantation, and can be confirmed by manual contrast injection during the procedure.
- An enlarged coronary sinus on echocardiography should raise suspicion of PLSVC which can be confirmed by administration of echo-contrast or agitated saline in the left arm.
- Although lead implantation through a PLSVC is technically feasible, difficulties in lead positioning may be encountered because of the acute angle between the origin of the coronary sinus and the tricuspid valve.
KEYWORDS
Persistent left superior vena cava, defibrillator, lead implantation, coronary sinus
INTRODUCTION
Persistent left superior vena cava (PLSVC) is a congenital venous abnormality which can be isolated or associated with congenital heart disease. It is typically characterized by an enlarged coronary sinus. The diagnosis can be incidental at the moment of a procedure such as central venous line or pacemaker implantation. We report the case of a patient with systolic heart failure undergoing implantation of a defibrillator lead through a PLSVC which was diagnosed at the moment of implantation.
CASE PRESENTATION
A 54-year-old man, known to have a restrictive muscular ventricular septal defect, presented with heart failure and atrial fibrillation with a rapid ventricular response. After decongestion and rate control, electrical cardioversion restored sinus rhythm. Treatment with guideline-directed medical therapy was initiated. The patient underwent left and right heart catheterization and coronary angiography. There was no significant coronary artery disease. However, there were elevated filling pressures with a wedge pressure of 29 mmHg and moderate postcapillary pulmonary hypertension with a mean pulmonary artery pressure of 40 mmHg.
The patient was moderately symptomatic (New York Heart Association class II). Because of the diagnosis of non-ischaemic cardiomyopathy with persistently depressed left ventricular function (ejection fraction 25%), the patient was referred for an implantable cardioverter-defibrillator (ICD). The ICD was implanted on the left side by puncture of the left subclavian vein. At that moment a PLSVC was found, confirmed by angiography with manual injection of contrast. The lead was manipulated through the coronary sinus into the apex of the right ventricle. The chest x-ray after the procedure confirmed correct lead position (Fig. 1). Transthoracic echocardiography (TTE) with injection of contrast bubbles by the left arm showed an enlarged coronary sinus (Fig. 2) and also raised suspicion of an atrial septal defect (ASD). Transesophageal echocardiography (TEE) confirmed an ASD type secundum of 6 mm and excluded an unroofed coronary sinus. Because the size of the ASD was small and the pulmonary hypertension was due to left-sided heart failure, conservative treatment for the ASD was proposed.
Figure 1. Chest x-ray after implantation of the implantable cardioverter-defibrillator (ICD) lead through the left subclavian vein with position in the apex of the right ventricle showing the acute angle at the level of the tricuspid valve
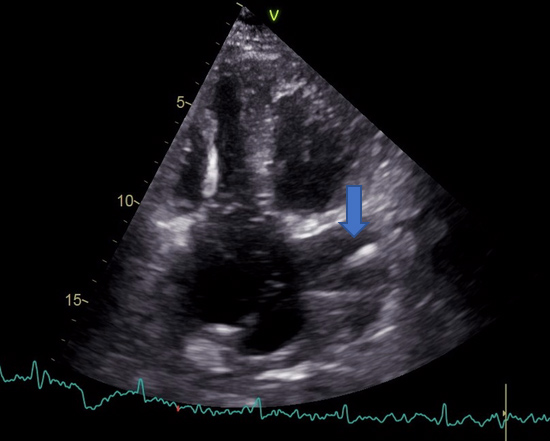
Figure 2. Transthoracic echocardiography showing the implantable cardioverter-defibrillator (ICD) lead in the dilated coronary sinus (blue arrow) and in the right ventricle
DISCUSSION
PLSVC is a venous anomaly with a prevalence of 0.3–0.5% in the general population and 1.5–10% in patients with congenital heart defects. The PLSVC is predominantly connected to the coronary sinus without haemodynamic abnormality and less often to the left atrium causing a right to left shunt either by direct entry into the left atrium or by an unroofed coronary sinus. Suspicion of a PLSVC is raised by the presence of an enlarged coronary sinus on TTE (>15 mm in adults) and can be confirmed by contrast echocardiography with intravenous administration of agitated saline or echo-contrast medium in the left arm, or by computed tomography or magnetic resonance imaging. The diagnosis can be incidental at the moment of a procedure such as pacemaker and ICD implantation.
The abnormal anatomy may lead to difficulties in lead fixation as it requires the lead passing through an acute angle between the orifice of the coronary sinus and the tricuspid valve [1]. Complications include lead dislodgement and pneumothorax [2]. Long-term follow-up after successful implantation has showed no difference in pacing parameters [3].
Preoperative or preprocedural detection and description of a PLSVC are important as well as description of an innominate vein. In case of periprocedural detection, a venous angiogram to detect an unroofed coronary sinus or direct entry into the left atrium is necessary. Although technically demanding, lead implantation through a PLSVC is feasible.