ABSTRACT
In this case, a 76-year-old female presented with 3–4 days of fever with no other localizing signs. Notably, she had had an untreated Fusobacterium bacteraemia approximately 8 weeks prior to admission. She underwent abdominal imaging which demonstrated a liver abscess and had percutaneous drainage of the same. Blood and pus cultures both grew Fusobacterium nucleatum, which is an unusual organism to be associated with a liver abscess, especially in an immunocompetent host with no risk factors for this condition. Interestingly, this patient did not have any history of dental work, instrumentation, liver function test (LFT) abnormalities and no extrahepatic source for the abscess. This case highlights the importance of having a high index of clinical suspicion for an occult source of infection and emphasizes the importance of following up on cultures even after discharge of a patient, since anaerobic infections such as those caused by Fusobacterium can have a largely indolent course.
LEARNING POINTS
- Fever of unknown aetiology with prior bacteraemia merits a thorough work-up for occult sources such as a localized abscess or malignancy, which can cause bacterial translocation.
- Fusobacterium and other anaerobic infectious agents should be considered in the context of an indolent disease course since they are slow-growing in cultures, and also, if the patient has risk factors such as immunosuppression, diabetes, poor oral hygiene and so on.
- It is important to have systems in place in hospitals to ensure follow-up for patients who may have a positive culture after discharge from hospital to confirm that the
KEYWORDS
Pyogenic liver abscess, Fusobacterium
CASE DESCRIPTION
A 76-year-old female with a past medical history of hypertension, chronic obstructive pulmonary disease and tobacco use disorder presented with complaints of fever, chills and night sweats for 3–4 days. She had chronic cough with mucoid non-purulent expectoration and no consolidation on a chest radiograph. She had no abdominal pain or urinary complaints, denied any loss of weight/appetite, an oral cavity examination showed no evidence of gingival disease. Her urine analysis was bland and her laboratory tests were unremarkable with no abnormalities in her blood count or liver function test results.
Of note, however, she had been hospitalized approximately 2 months prior to presentation with dizziness, confusion, upper respiratory symptoms and low-grade fever. Blood cultures drawn during this admission grew Fusobacterium, but the patient was discharged before the results were obtained, and hence, she was never treated. In view of this history, blood cultures were redrawn, and the patient was empirically started on broad-spectrum antibiotics; vancomycin (15 mg/kg every 12 hours), cefepime (2 g every 12 hours) and metronidazole (500 mg every 8 hours) for 4 days.
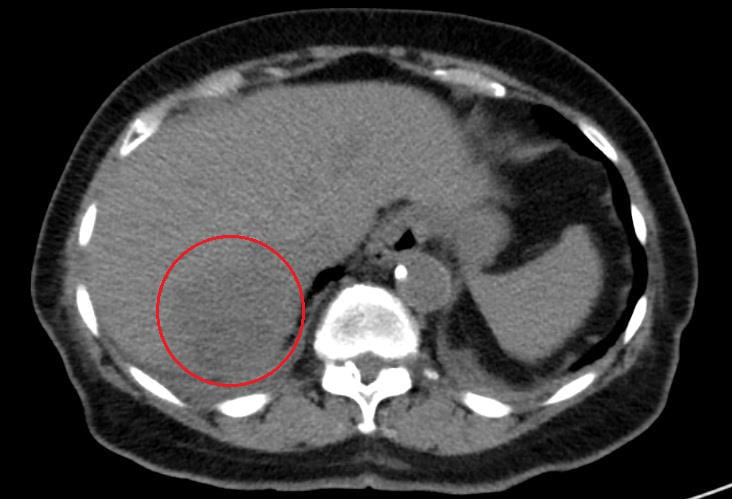
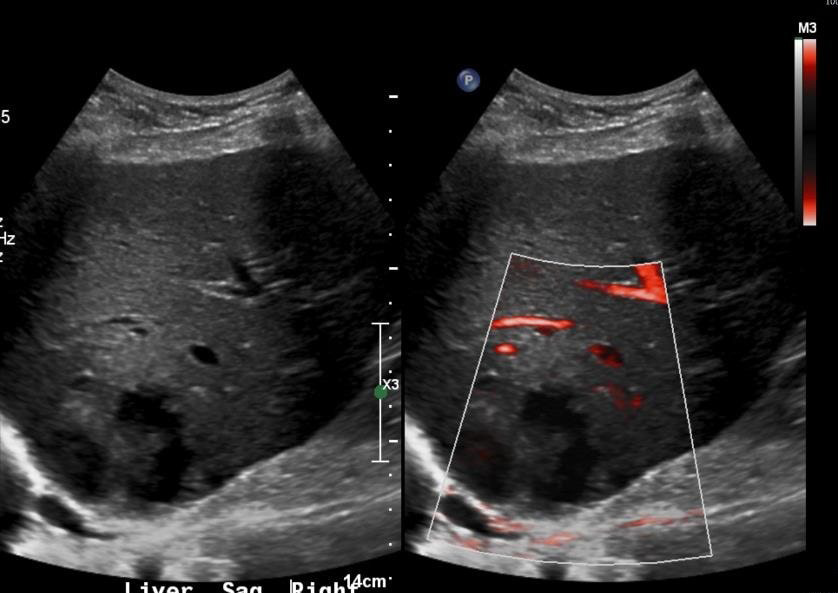
In view of the persistent fever in this elderly female, abdominal imaging was ordered to look for evidence of an occult focus of infection versus occult abdominal malignancy. A CT scan showed a hypodense lesion in the right lobe of the liver (Fig. 1) and colonic diverticulosis with no evidence of biliary ductal dilation or acute diverticulitis. Further characterization with ultrasound showed a complex solid and cystic mass with an appearance most characteristic of a liver abscess (Fig. 2) There was normal flow in the portal and hepatic vasculature.
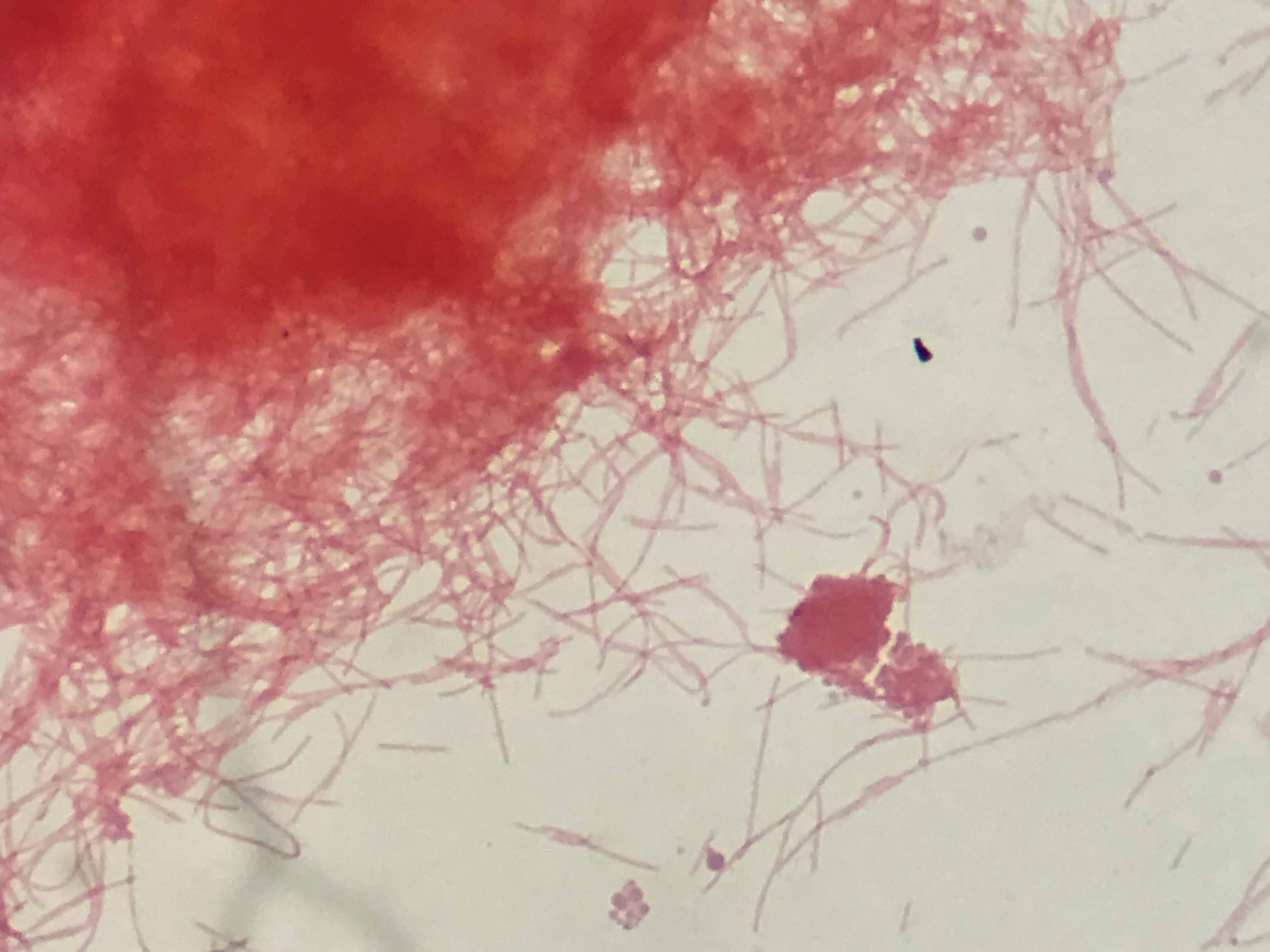
The patient underwent ultrasound-guided percutaneous drainage of the abscess. Blood culture and pus drained from the liver abscess eventually grew Fusobacterium nucleatum (Fig. 3).
Figure 1. A rounded 5.8×5 cm hypodense lesion with a thick surrounding rim in the posterior segment of the right lobe of the liver
Figure 2. A complex isoechoic lesion with few cystic foci, no internal vascularity and mild peripheral vascularity located in the peripheral posterior hepatic lobe corresponding with the mass identified on CT
Figure 3. Spindle-shaped Gram-negative rods
The patient had negative HIV and hepatitis testing and there was no evidence of valvular vegetation on a transthoracic echocardiogram. A review of her history showed no risk factors for parasitic infection with agents such as Strongyloides.
Based on the culture which was positive for Fusobacterium and negative for β-lactamase, the antibiotics were de-escalated to oral amoxicillin (500 mg every 8 hours) to complete a total 4-week course. The patient was discharged with the drain in situ and provided with instructions and suppliers for appropriate drain care. She underwent drain removal 9 days post-discharge, after an abscessogram demonstrated resolution of the abscess and the drain output was noted to be less than 10 cc over 24 hours.
The patient also followed up for repeat blood cultures 1 week after completion of the antibiotic course to document clearance of the bacteraemia. She was counselled to undergo a formal dental evaluation and a colonoscopy procedure as an outpatient, since these assessments could perhaps identify the possible source of development of Fusobacterium bacteraemia.
DISCUSSION
Liver abscesses can be of 2 major types; pyogenic or amoebic. A pyogenic liver abscess refers to an encapsulated collection of purulent material. It is often seen in the right lobe of the liver since it is larger in size and has a greater blood supply compared to the left lobe or the caudate lobe. The mechanisms for liver abscess formation include dissemination via the portal vein, secondary to biliary tract disease or from haematogenous spread. The typical risk factors associated with a liver abscess include diabetes mellitus, immunosuppression, intra-abdominal malignancy or a history of biliary procedures [1, 2]. A pyogenic liver abscess is cryptogenic when no extrahepatic source is identified. Cryptogenic abscesses are usually solitary whereas multiple abscesses are seen with biliary causes. It appears that cryptogenic abscesses are associated with earlier defervescence, a better response to antibiotics and shorter hospital stays. Cryptogenic liver abscesses appear to have a link with colonic polyposis and increased risk of colon cancer [1, 3]. The most common laboratory abnormalities seen with pyogenic liver abscesses include hypoalbuminaemia, elevated gamma-glutamyltransferase (GGT), increased alkaline phosphatase (ALP) and leucocytosis. The typical appearance of an abscess on imaging is central necrosis and a surrounding hypo/hypervascular rim, which can be layered. Organized abscesses may have an appearance that can mimic solid tumours. Liver abscesses are also associated with portal/hepatic vein thrombosis and it is useful to look for evidence of the same as this may necessitate anticoagulation therapy [3].
Management of a liver abscess involves percutaneous drainage and antibiotic treatment. Surgical intervention should be considered in cases where the size of the abscess is greater than 5 cm, there are gas-forming organisms or in cases of biliary fistulization. The duration of antibiotic treatment ranges from 2–6 weeks, depending on the clinical severity and response to therapy [1]. Usually, pyogenic liver abscesses are polymicrobial and common pathogens isolated are Escherichia coli, Klebsiella, viridans streptococci, Bacteroides, Proteus, Enterobacter, Pseudomonas, Staphylococcus and Citrobacter, among others.
Fusobacterium is an uncommon cause of a liver abscess [4]. Fusobacterium encompasses many different species and the most common pathogen among them is Fusobacterium necrophorum. Fusobacterium nucleatum is a rare pathogen. The annual incidence of Fusobacterium infections is 0.6–3.5 cases per 100,000 people. In previously described cases of Fusobacterium liver abscess, the following sources and risk factors have been identified: septic thrombophlebitis of the jugular veins, which is also referred to as (the eponymously named) Lemierre’s syndrome [4], chronic denture use, oropharyngeal infection and sigmoid diverticulitis causing bacterial translocation and seeding [4, 5].
This patient had no evidence of gingival disease on examination. The patient did not undergo any dental imaging such as an orthopantomogram since that was not available on an inpatient basis. However, diverticulosis was noted on imaging. There is limited evidence for the association of diverticulosis with development of a liver abscess. Based on a review of the literature on cases it seemed reasonable to advise the patient to undergo an outpatient dental evaluation as well as a colonoscopy, which was carried out [6, 7].